When Institutional Authority Collapses, Relational Trust Networks Decide
The Hidden Physics of Vaccine Belief
When Institutional Authority Collapses, Relational Trust Networks Decide
The Hidden Physics of Vaccine Belief

In 1964, the United States created the Advisory Committee on Immunization Practices (ACIP) to do something deceptively simple, translate science into protection. For decades, it worked. Its authority rested on three pillars, scientific expertise, institutional independence, and public trust. In 1979, the Belmont Report gave that authority an ethical foundation; respect for persons, beneficence, and justice. And yet, for many Americans, justice had already been broken.
From 1932 to 1972, the US Public Health Service conducted what became known as the Tuskegee Study. In 1997, President Bill Clinton issued a formal apology. But apology does not erase history; it redistributes it, into memory, into behavior, and into the quiet, often unspoken calculations people make when deciding whether to trust what they are told. This inheritance has come to be understood in community discourse as the “Legacy of Our Fathers”, not as an excuse for disengagement, but as a demand that systems of care be worthy of trust, accountable in practice, and just in outcome
Long before Advisory Committee on Immunization Practices (ACIP), and long before its current unraveling, Black professionals confronted a different kind of institutional failure. When excluded from the American Medical Association, they formed the National Medical Association in 1895. Black nurses organized in 1908, and Black dentists established the National Dental Association in 1913. These were not symbolic acts; they were structural responses. When dominant institutions excluded, communities built parallel systems capable of carrying life. What is often described today as “community engagement” was, in fact, something far more foundational, survival infrastructure, durable systems designed to function when formal governance fails
The African American Diabetes Association (AADA) stands within this lineage, not as an alternative, but as a continuity mechanism, translating evidence into culturally grounded action, reaching populations systematically underserved, and sustaining care in the absence of institutional trust. This is the deeper pattern, when legitimacy collapses, continuity does not emerge spontaneously, it is already present, or it is not.
The COVID-19 pandemic provided a real-time stress test of this architecture. It did not create distrust, it revealed the systems that could operate despite it. In that moment, a simple question emerged, who can actually deliver trust under pressure? The answer was visible in barbershops and beauty salons, where initiatives such as Shots@Shop transformed trusted chairs into points of care. These were not outreach efforts or messaging campaigns, they were conversion infrastructures, moving individuals from hesitation to dialogue, from dialogue to decision, and from decision to vaccination. Their effectiveness did not arise from communication strategy alone, but from relationship density built over years.
What we are witnessing now, in the wake of ACIP’s erosion, is not simply a breakdown of authority. It is a network phenomenon. In earlier work with Patrick Grimm, we demonstrated that beliefs do not move through populations as facts, they move as relational signals carried by trusted nodes. Individuals update beliefs not based solely on evidence, but on who they trust, and who those people trust. Over time, this produces belief polarization: groups exposed to the same information move further apart rather than closer together, as each filters through its own network, discounts external sources, and reinforces internal agreement. Truth does not circulate freely in such systems; it travels along trust pathways.
ACIP once functioned as a bridging institution, a shared reference point across networks. When that bridge weakens, networks decouple, trust localizes, and beliefs diverge. This is not speculative; it is precisely what the Grimm–Thomas models predict. It also explains why simply increasing the volume of information or amplifying expert consensus fails to correct the problem. In a polarized system, more information does not produce agreement, central authority does not ensure uptake, and evidence does not guarantee legitimacy. Without trusted pathways, information does not propagate, it ricochets within bounded networks.

The HAIR Network operates on a different principle. It does not attempt to override polarization from above, it reconfigures the structure of the network from within. By embedding health engagement in barbers, stylists, and other trusted community nodes, it alters the conditions under which beliefs are formed. In network terms, it increases overlap between clusters, reduces echo chamber isolation, and restores pathways for convergence. This is not outreach, it is network design.
If we take the Grimm–Thomas framework seriously, the implications are clear. In a fragmented system where professional societies act without integration into community networks, belief polarization will accelerate, vaccine uptake will diverge, misinformation will spread more effectively, and disparities will widen. In a system that relies solely on centralized messaging campaigns, behavior change will remain minimal, and beliefs will harden. But in a system where professional guidance is integrated with community-embedded trust infrastructure, where trusted nodes function as co-producers rather than messengers, the model predicts convergence across networks, increased completion of care, resilience to future shocks, and measurable reductions in disparities. The central insight is stark, the model does not predict that truth prevails, it predicts that the network with the strongest trust pathways determines outcomes.
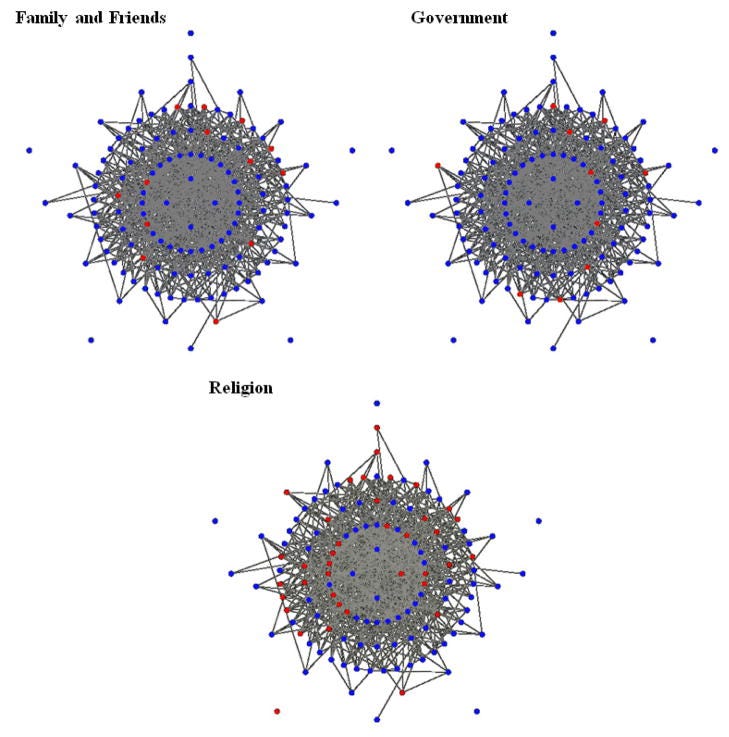
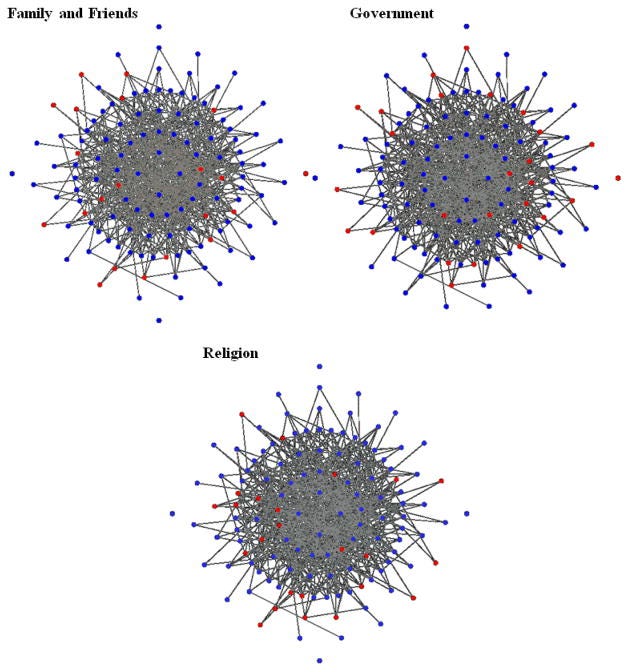
Fig. 3
Trust levels in information sources in the White community. Blue = positive trust. Red = Distrust
Current policy debates remain incomplete because they focus on federal authority and professional societies while overlooking the layer that has consistently determined real-world outcomes, relational infrastructure. These networks are local, dense, trusted, and persistent. They do not emerge during crises, they are revealed by them.
If legitimacy is to be rebuilt, public health must align three layers: 1) federal science, when credible, 2) professional synthesis, when trusted and 3) community implementation, where belief actually lives. Remove the third layer, and the system fails, not occasionally, but predictably.
We did not arrive at this moment unprepared. For many communities, institutional reliability has always been uncertain. So different systems were built, quietly, relationally, and durably. Systems designed not for ideal conditions, but for moments like this.
When institutional trust collapses, outcomes are not determined by authority. They are determined by the networks that carry belief, and the relationships that sustain them.